What Is Hyperbaric Oxygen Therapy ?
As a plastic surgeon, I am often asked how I can recover from surgery faster and better. One of the complementary therapies I often refer to is hyperbaric oxygen therapy (Hyperbaric Oxygen Therapy, or HBOT). Simply put, HBOT allows patients to inhale about 95% pure oxygen in a special pressurized chamber.

Rationale
You might think, isn’t it just oxygen? What’s so special about it? Actually, it’s not. In a hyperbaric oxygen chamber, the pressure will be 1.5 to 3 times higher than the atmospheric pressure we usually find ourselves in. Inhaling pure oxygen in such a high-pressure environment is not a simple “more oxygen.
Its core principle is that high pressure can make more oxygen dissolved into our blood. We know that oxygen is mainly transported by red blood cells, but HBOT allows oxygen to be dissolved directly into the plasma. This is like a cup of water. The sugar that can be dissolved at normal pressure is limited, but if you stir under pressure, you can dissolve more. When the plasma carries far more than normal levels of oxygen, the oxygen can more effectively penetrate into tissues and cells that are usually hypoxic and hypoxic.
What does this mean for wound healing after plastic surgery? This means that damaged tissues, edematous sites, and even transplanted flaps can get a better supply of oxygen. Adequate oxygen is the key “fuel” for a series of healing processes such as cell repair, collagen synthesis, and angiogenesis “. With it, the recovery of tissues will be significantly faster and the risk of infection will be reduced. Of course, this is only a theoretical basis, and the actual effect needs to be judged according to the specific situation.

A. Scientific Overview of the Healing Process
From my experience with thousands of surgeries, healing after plastic surgery does not happen overnight, but is a subtle and interlocking biological process that can be roughly divided into 3 key stages:
- Inflammatory phase
This is the phase initiated immediately after surgical trauma and usually lasts for several days. During this period, we observe the body’s spontaneous defense and clearing mechanisms. White blood cells quickly build up in the surgical area and act as efficient scavengers, engulfing damaged cells, bacteria and foreign bodies. Patients will feel local redness and slight pain, which is not a bad thing, but the body is actively for the follow-up tissue repair “clean up the battlefield” of the normal physiological response. - Proliferation phase
Usually within a few days to a few weeks after surgery, the proliferative phase will quietly open. This is the most active period of tissue regeneration. Fibroblasts-the “architects” of our bodies-synthesize collagen in large quantities, and new capillaries are rapidly formed to deliver valuable oxygen and nutrients to the healing area. At this stage, we can see that the wound gradually converges and granulation tissue begins to fill the gaps, which is a sign of the initial formation of new tissue. - Reshaping period
This is a long and crucial phase that can last for months and in some cases more than a year. During the remodeling period, the disorganized collagen fibers formed in the early stage will continue to reorganize, arrange and mature. The scar tissue will gradually become softer and flatter, and the color will gradually fade. This process requires a great deal of patience, because the final quality and aesthetics of the scar depends to a large extent on the fine adjustment of this stage. We often say that the final appearance of scars is the result of a combination of time and biology.
B. common challenges after surgery
Despite our best efforts to use the best surgical skills, there are always some predictable challenges to the healing process. These are all the situations that I repeatedly encounter in my daily outpatient service:
- Swelling and Bruising:
This is a phenomenon experienced by almost all patients after plastic surgery. Tissue is damaged during surgery, resulting in increased capillary permeability, fluid leakage, and sometimes subcutaneous hemorrhage with vascular rupture. These can cause local swelling and bruising. Although it usually subsides gradually within a few weeks, there are significant individual differences in its duration and extent. We will help patients reduce these discomfort through cold compresses, proper compression and postural management. - Pain:
Postoperative pain is the body’s natural response to trauma and is almost inevitable. My team will prescribe the appropriate pain medication based on the patient’s specific situation to ensure that the patient feels maximum comfort during the recovery period. With the advancement of healing, the pain will gradually reduce, which is a positive signal for the body to recover. - hematoma:
Occasionally, blood may accumulate under the surgical area to form a hematoma due to incomplete hemostasis of blood vessels during or in the early postoperative period. Small hematomas may be self-absorbed, but larger hematomas may require prompt drainage to avoid compromising healing and final outcome. This is one of the key points of our close observation after surgery. - Risk of infection:
Although uncommon, any invasive procedure carries a potential risk of infection. Therefore, we always put aseptic practice in the first place. Depending on the type of surgery and the patient, antibiotics are sometimes used prophylactically to minimize the chance of infection. We emphasize the importance of postoperative wound care and will instruct patients on how to recognize early signs of infection. - Scarring:
Scars are an inevitable product of tissue healing, but our goal is always to minimize them and make them as hidden and beautiful as possible. The final shape of the scar is influenced by many factors, including the patient’s genetic predisposition, the surgeon’s fine suture technique, and the patient’s standardized postoperative care. We fully assess the patient’s scar physique preoperatively and provide a detailed postoperative scar management protocol.
C. Oxygen in Healing “Secret Weapon”
- Now, I want to draw your attention to a factor that may be underestimated in daily discussions, but plays a vital role in the physiological healing process-oxygen. In my opinion, sufficient oxygen is simply the “life fuel” for cell repair and tissue regeneration, and its importance cannot be overemphasized.
- cell repair and proliferation of the driving force:
Whether it is the elimination of necrotic tissue by leukocytes in the inflammatory phase or the synthesis of collagen by fibroblasts in the proliferative phase, all these complex cellular activities require a continuous and large supply of oxygen to maintain their vigorous metabolism. Without enough oxygen, the function of these key cells will be greatly reduced, which directly affects the healing efficiency. - the necessary conditions for collagen synthesis:
Collagen, the basic scaffold for building new tissue and giving wound strength, requires an enormous amount of oxygen during its synthesis. Without sufficient oxygen, the crosslinking and maturation of collagen will be hindered, which will directly affect the strength of the wound tissue and may lead to poor quality scar healing. - Key support for angiogenesis:
During the proliferative phase, the body actively initiates the process of “angiogenesis”, that is, the formation of a new capillary network to transport more blood, oxygen and nutrients to the healing area. This is a highly oxygen-consuming biological process. If the local oxygen supply is insufficient, angiogenesis will become delayed or even blocked, which will undoubtedly slow down the overall healing process and may affect the healthy growth of new tissue.

How Does Hyperbaric Oxygen Therapy Accelerate Recovery After Plastic Surgery?
Throughout my years of orthopedic practice, I have been exploring ways to optimize my patients’ recovery. Hyperbaric oxygen therapy (HBOT) is one of them, it is one kind of very worthy of our attention adjuvant therapy. In simple terms, HBOT allows patients to breathe 100 percent pure oxygen in a controlled, pressurized environment. Under this non-physiological high-pressure condition, oxygen can enter the plasma in large quantities in a physically dissolved manner, significantly increasing the oxygen supply to various tissues of the body (especially those areas that are damaged by surgery and have limited blood supply). This is a crucial part of the healing process after our plastic surgery.
A. Reduce swelling and bruising: Any surgery, even the most delicate plastic surgery, will cause a certain degree of tissue trauma, postoperative local swelling and bruising is almost inevitable. My understanding is that hyperbaric oxygen can reduce capillary permeability and tissue fluid leakage by improving microcirculation and promoting moderate contraction of small blood vessels, which directly helps to reduce postoperative edema. At the same time, a more adequate supply of oxygen can speed up cell metabolism, help to remove local accumulation of fluid and metabolic waste, so as to more quickly subside bruises. From clinical observations, patients who received HBOT generally had a better rate of resolution of swelling and bruising.
B. Promotes Wound Healing: There is no doubt that oxygen is essential for cell survival, metabolism and tissue regeneration. Under the hyperoxic environment provided by HBOT, the oxygen tension at the wound site is significantly elevated. This hyperoxic environment is like injecting a cardiotonic into tired cells, which directly activates the activity of fibroblasts-you know, these cells are our main force in producing collagen, building new tissue, and repairing wounds. At the same time, sufficient oxygen also accelerates the migration and proliferation of epidermal cells, as well as the formation of new blood vessels (angiogenesis), which lays a solid biological foundation for effective wound healing. This is very attractive to our plastic surgeons who are looking for perfect healing results.
C. Pain Reduction: Pain after surgery is a common challenge experienced by patients. I have observed that hyperbaric oxygen, through its anti-inflammatory effect, reduces the inflammatory response in the surgical area, thereby reducing the stimulation of inflammatory mediators to nerve endings, thereby indirectly relieving pain. In addition, if the pain is related to ischemia or tissue edema compression, the effect of hyperbaric oxygen to improve oxygen supply and reduce edema can also have a positive impact. Although the direct effect of hyperbaric oxygen on nerve repair is still under study, from my patient feedback, most patients receiving HBOT generally believe that the postoperative pain has been reduced and the need for analgesic drugs has also been reduced.
D. Reduce infection risk: Although the aseptic operation standards in our plastic surgery operating room are extremely high and the incidence of postoperative infection is relatively low, once it occurs, the consequences are often disastrous. The advantage of hyperbaric oxygen is its direct inhibition of certain anaerobic bacteria-bacteria that simply cannot survive in an oxygen-rich environment. More importantly, sufficient oxygen can significantly enhance the phagocytosis and bactericidal ability of white blood cells (especially neutrophils and macrophages) in our body, and improve the body’s own immune defense mechanism. From the point of view of preventing infection, I think it is very beneficial to use it as a auxiliary means.
E. Optimize scar quality: The scar is the “mark” of plastic surgery. As doctors, we always want it to be as unnoticeable and unobtrusive as possible. Hyperbaric oxygen is thought to regulate the inflammatory response and help us avoid the formation of abnormal scars (such as hypertrophic scars or keloids) by optimizing the collagen synthesis and remodeling process. My understanding is that it can promote healthy type I collagen production and guide the collagen fibers to arrange more regularly and orderly, which makes the final scar flatter, softer, and the color is closer to the surrounding normal skin. Achieve a better aesthetic effect.
F. Improving flap and graft survival (for more complex plastic surgeries): For those complex reconstructive or plastic surgeries that involve flap grafting or tissue grafting, the blood supply of the tissue is the life line that determines success or failure. When the skin flap or graft tissue shows signs of hypoxia or even near necrosis due to insufficient blood supply, hyperbaric oxygen therapy can dramatically increase its local oxygen tension. It can save these tissues that are facing ischemia-reperfusion injury or on the verge of necrosis to a certain extent, thus significantly improving the survival rate of flaps and transplanted tissues. HBOT is often a powerful adjunct strategy that I consider when dealing with complex, high-risk reconstruction cases.
G. My clinical insights and case sharing: There are indeed some cases in my career that have impressed me with the role of hyperbaric oxygen in rehabilitation after plastic surgery. I once had a patient who underwent a more complicated abdominal wall surgery. Due to individual differences and some incidental factors in the initial stage, her initial postoperative recovery was not satisfactory, and local swelling and bruising were more obvious than other patients. Her recovery trajectory changed positively after I advised her to try adjunctive hyperbaric oxygen therapy. I noticed that the swelling in her surgical area quickly subsided after a few HBOT treatments, and the bruising faded faster than I originally expected.
What Types Of Plastic Surgery May Benefit From Hbot?
A. facial plastic surgery: blepharoplasty, skin lift, rhinoplasty.
Facial surgery is often particularly sensitive to swelling and bruising because they directly affect the patient’s appearance and sociability. After blepharoplasty, hyperbaric oxygen can help reduce periocular edema and allow patients to “see people” faster “. After skin lift surgery, especially deep tissue reduction, the blood supply of skin and subcutaneous tissue may be affected. HBOT can help improve local circulation and reduce complications. After rhinoplasty, the healing of cartilage and bone requires a lot of oxygen, and hyperbaric oxygen may accelerate the healing process and reduce postoperative swelling.
B. breast plastic surgery: breast augmentation, breast lift, breast reduction.
For breast augmentation surgery, if there is a risk of capsular contracture, although evidence is still accumulating, some studies suggest that HBOT may help reduce the inflammatory response. Breast lift and breast reduction surgery involves the removal and remodeling of a large amount of skin and glandular tissue. Hematoma and infection are complications that need to be monitored. Hyperbaric oxygen can provide support in this regard and help the tissue recover more quickly.
C. body shaping: liposuction, abdominal plastic surgery.
After liposuction, the local tissue will form a cavity and may be accompanied by significant swelling and bruising. Hyperbaric oxygen can accelerate fluid absorption and tissue repair in these areas. Abdominal surgery (Tummy Tuck) is a large-scale tissue separation and suture, and sometimes blood supply is a challenge. HBOT can effectively promote tissue healing and reduce the occurrence of skin complications, such as necrosis, after such surgery.
D. Complex reconstructive surgery.
This includes some complex tissue flap transplants resulting from trauma, tumor removal, or congenital malformations. In these cases, the survival of the transplanted tissue flap is critical. I have encountered some complicated cases in which hyperbaric oxygen therapy has significantly improved flap survival and reduced the risk of postoperative infection and tissue necrosis. It’s like sending a kind of “life gas” to tissues that are on the verge of hypoxia “.
Safety Considerations And Precautions Of Hyperbaric Oxygen Therapy
As a plastic surgeon, I know that every patients are most concerned about safety and final recovery. Therefore, when we consider hyperbaric oxygen therapy (HBOT) in the scope of postoperative rehabilitation, it is particularly critical to understand its safety, applicability and potential risks. This is not only a technical operation, but also related to the well-being of patients.
HBOT: Who is suitable?Who is not?
First, let’s be clear: hyperbaric oxygen therapy is not a universal “panacea”. In my clinical practice, I will be very careful to assess the individual situation of the patient.
- Applicable people: HBOT is usually a very useful adjunct for patients who need to accelerate tissue healing, effectively reduce postoperative swelling and pain, and prevent infection after plastic surgery. For example, I have included HBOT in the discussion of post-operative recovery options for liposuction, abdominal wall surgery, various types of breast surgery (including breast augmentation or breast reconstruction), and complex facial lift surgery. By providing a high concentration of oxygen to the damaged tissue that far exceeds the regular environment, it can significantly promote cell repair, collagen production, and the formation of new blood vessels, thereby optimizing the overall recovery process.
- Contraindications: I would emphasize, however, that there are clear contraindications to hyperbaric oxygen therapy. In any case, if patients have the following conditions, they must tell us the truth before treatment, because it is related to their life safety:
- Untreated pneumothorax: an absolute contraindication. In a high-pressure environment, pneumothorax can deteriorate rapidly with disastrous consequences.
- Recent chest surgery history: pulmonary lobectomy, etc., need detailed evaluation of lung function and healing, high risk.
- Certain serious lung diseases: advanced chronic obstructive pulmonary disease (COPD), severe bullae, etc., these conditions may lead to lung damage under high pressure.
- Failure to effectively balance ear pressure or sinus pressure disease: patients in the pressure process will feel severe discomfort, and even cause damage.
- Active seizure history: possible reduction of seizure threshold in high pressure environment.
- are using certain chemotherapy drugs: bleomycin (Bleomycin), for example, and hyperbaric oxygen may have adverse interactions with these drugs.
- Pregnancy: This treatment is generally not recommended for pregnant women out of the utmost caution, although there is currently no conclusive evidence that HBOT is harmful to the fetus.
In my daily work, careful screening of the patient’s medical history is the first and most important step before HBOT. If there are any even minor doubts, we will resolutely choose other more secure adjuvant treatment options. After all, the safety of patients is my primary responsibility.
HBOT treatment process
Many patients will be curious, a hyperbaric oxygen therapy is what kind of experience? In fact, this is far less complex than imagined.
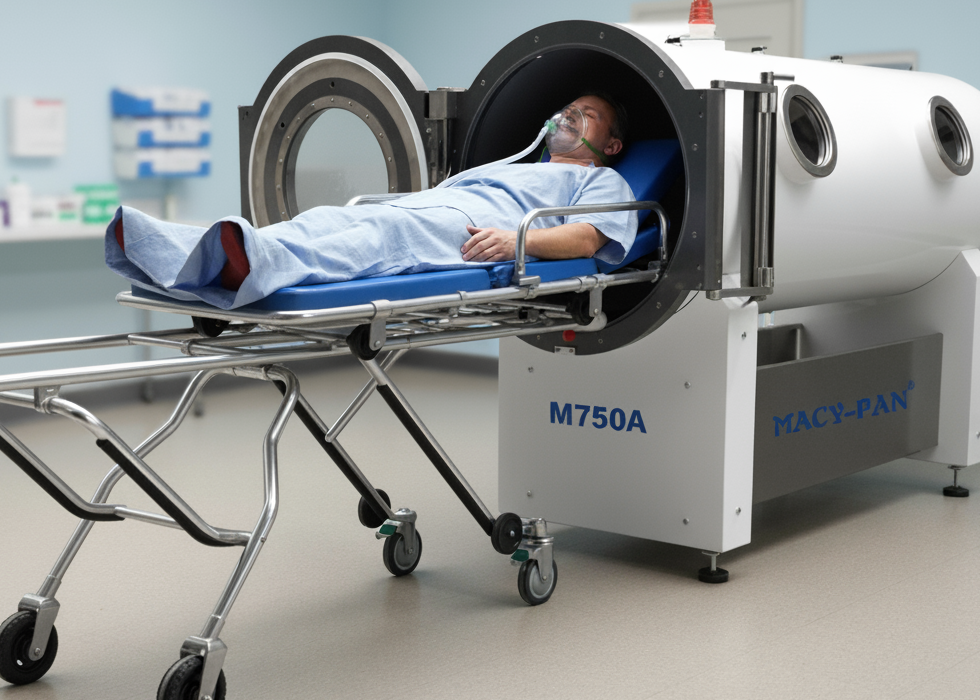
When you enter the hyperbaric oxygen chamber, the pressure in the chamber will gradually increase, simulating an environment similar to diving deeper into the water. During this pressurization process, you may feel a little stuffy in your ears, which is very similar to the feeling when taking off and landing in an airplane or ascending in the mountains. This is a completely normal physiological response, and ear pressure can usually be effectively balanced by simply swallowing, yawning, or pinching the nose to exhale gently (Valsalva action).
You will usually lie or sit comfortably throughout the treatment. The cabin is quiet, so you can choose to read, close your eyes, or even watch our TV programs to relax. The duration of a single treatment typically lasts from 60 to 90 minutes. I often tell my patients that this time can be thought of as an exclusive “body charging station”, allowing the body to obtain deep repair and energy supplement in an oxygen-rich environment.







No Comment! Be the first one.