Dr. Jonathan Reed, MD, PhD
Medical Advisor, MACY-PAN
Dr. Jonathan Reed is a board-certified specialist in hyperbaric and regenerative medicine with over 15 years of clinical and research experience. He currently serves as the Medical Advisor for MACY-PAN, collaborating with engineers to optimize hyperbaric chamber design for patient safety and clinical effectiveness.
Dr. Reed has published multiple papers on tissue oxygenation and wound healing and works closely with surgeons to integrate HBOT into postoperative recovery protocols. His mission is to bridge medical science with innovative technology, making advanced oxygen therapy accessible and effective for patients worldwide.
In the field of modern plastic surgery, the success of surgery has long depended not only on the doctor’s technique, but also on the quality of postoperative recovery. How to make tissue heal faster, reduce swelling and infection, and make scars softer and more natural has always been the focus of surgeons and patients. In recent years, Hyperbaric Oxygen Therapy (HBOT) has gradually become a high-profile adjuvant therapy in postoperative rehabilitation.
Whether it’s facial surgery, breast reconstruction, liposuction or flap transplantation, HBOT has been shown to “speed up” surgical recovery by improving tissue oxygenation, reducing inflammation and promoting repair “. This article will give you an in-depth understanding of how HBOT works, scientific evidence, clinical applications and safety instructions to help you fully understand how this cutting-edge therapy can help postoperative recovery.

What Is Hyperbaric Oxygen Therapy (HBOT)?
At normal atmospheric pressure, the oxygen we inhale is mainly transported by hemoglobin binding. But in a high-pressure environment, pure oxygen not only saturates hemoglobin, but more importantly, it can significantly increase the amount of dissolved oxygen in the blood. This oxygen-rich plasma can directly reach tissues with damaged blood vessels and insufficient blood flow, which is essential for postoperative healing.
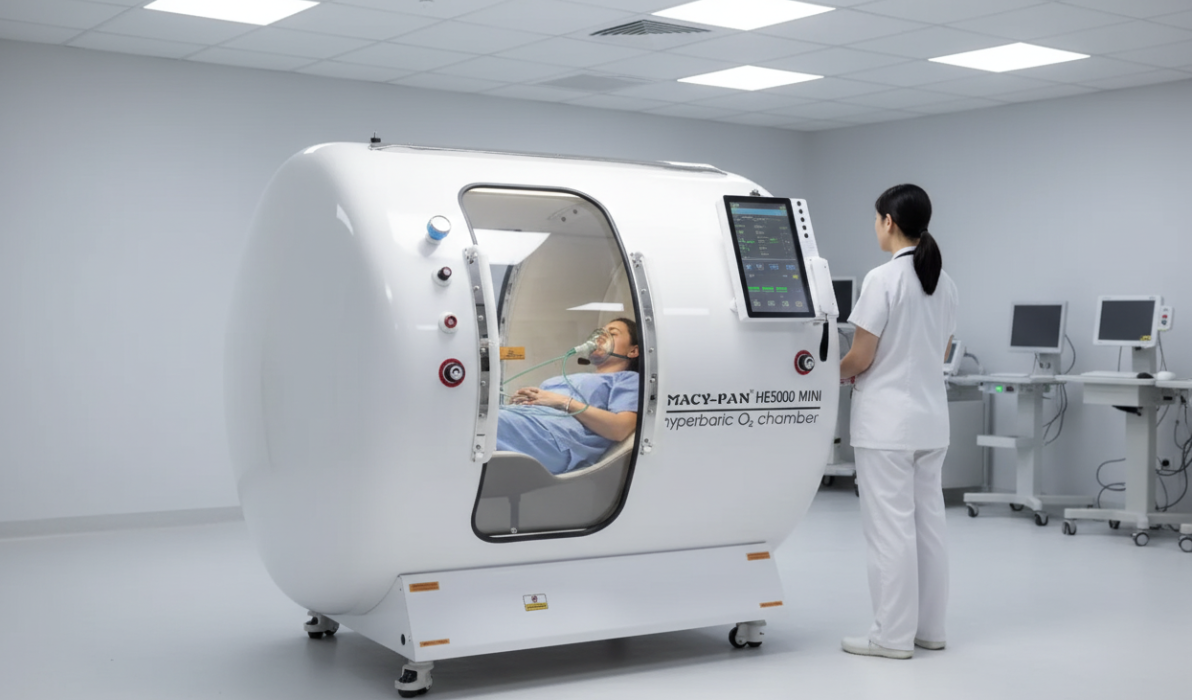
How exactly does this “hyperbaric oxygen chamber” work? It is actually a closed chamber that can precisely control the pressure inside and deliver pure oxygen. The patient will lie comfortably inside and breathe pure oxygen through a mask or hood.
Historically, hyperbaric oxygen therapy is not new. Its initial application can be traced back to the 17th century, but the importance and development of modern medicine was mainly during World War II, when it was used to treat diving disease, that is, decompression sickness. Later, with the deepening of research, we found that it has a significant effect in the treatment of carbon monoxide poisoning, chronic wounds, infections, and even burns and other indications. Now, it is also being increasingly used for recovery after plastic surgery.
In terms of mechanism of action, the effects of high concentrations of oxygen on cells and tissues are multifaceted. It can promote angiogenesis, increase collagen synthesis, fight infection, and reduce edema and inflammation. These are key factors in accelerating tissue repair and promoting wound healing.
How HBOT Helps the Body Heal After Surgery?
Plastic surgery, whether reconstructive or cosmetic, lies at its core in fine tissue remodeling and healing. The speed and quality of postoperative recovery directly affect the final effect. And hyperbaric oxygen therapy, it is through a variety of physiological mechanisms, for our body to provide an “accelerated healing” environment.
Enhanced oxygen supply:
This is the most direct and important role of HBOT. Imagine that the tissues after surgery, especially those areas that have been stripped and transplanted, may be damaged and the blood flow supply is not as good as before. Lack of oxygen is the enemy of healing. In the hyperbaric chamber, the patient inhales 100 percent pure oxygen at 2-3 atmospheres. This high pressure allows oxygen to be dissolved in the plasma in an amount 10-15 times that of normal pressure. This means that even those areas with restricted blood flow, or even complete occlusion of blood vessels, can be nourished by the oxygen carried by the plasma. This is essential for the “Hyperbaric Oxygen Therapy After Plastic Surgery” because plastic surgery often involves delicate flaps and skin grafts, which are extremely demanding for oxygen supply. Adequate oxygen is the basis for cell metabolism, energy production and tissue repair.

Reduces inflammation and edema:
In the early postoperative period, inflammation and edema are almost inevitable. This not only causes pain, but also compresses blood vessels, further aggravating local hypoxia. HBOT can effectively reduce inflammation and tissue edema by constricting blood vessels (but not affecting oxygen delivery, as it is supplemented by plasma oxygen) and reducing vascular permeability. The reduction of edema means that tissue pressure is reduced, blood circulation is improved, and pain will naturally be relieved. The rapid regression of postoperative edema is one of the significant improvements that patients can directly feel.
Promoting Angiogenesis:
In the long term, tissue healing requires the establishment of a new vascular network to provide a continuous blood supply. HBOT can stimulate the proliferation and migration of endothelial cells and promote the formation of new capillaries, which is often referred to as angiogenesis. This is of decisive significance for those areas that need long-term blood supply support, such as large-area flap transplantation and fat filling. Without good vascularization, these tissues are difficult to survive and be healthy for a long time.
Promote collagen synthesis:
Collagen is a key structural protein for wound healing and scar formation. The hyperoxic environment activates the fibroblasts, encouraging them to synthesize more collagen. More importantly, hyperbaric oxygen can also help collagen to cross-link and make its arrangement more orderly, which is very beneficial to reduce the formation of abnormal scars and improve the quality and aesthetics of the final scar. In the long run, this undoubtedly improves the overall effect of plastic surgery.
To fight infection:
Infection is always a potential risk after plastic surgery. Hyperbaric oxygen has a direct inhibitory and killing effect on some anaerobic bacteria, such as Clostridium perfringens. At the same time, the high oxygen environment can also enhance the bactericidal ability of white blood cells and improve the body’s own immune defense mechanism, thereby significantly reducing the risk of postoperative infection.
Scientific Evidence and Benefits After Plastic Surgery

In my many years of clinical practice, and under the continuous attention of the latest medical advances, the application of hyperbaric oxygen therapy (HBOT) in the recovery after orthopedic surgery has indeed demonstrated convincing scientific evidence and significant benefits. I personally have a very positive view of this, because it can actually help patients recover faster and better.
Specific application scenarios of HBOT
Hyperbaric oxygen therapy is not a panacea, but it has its unique advantages in the field of plastic surgery, based on physiological principles. In particular, we focus on its performance in the following key application scenarios:
- Skin grafting and flap survival: This is probably one of the most widely known applications of HBOT in plastic surgery. When faced with complex flap transplantation, especially those cases where blood supply may be impaired, HBOT can significantly improve microcirculation in the ischemic area by increasing tissue oxygenation, thereby increasing flap survival. I have seen many cases where HBOT intervention can often turn the situation around when there are signs of bruising on the edge of the flap.
- Reduction of complications after breast reconstruction: Breast reconstruction, especially when using autologous tissue flap for reconstruction, may face postoperative complications such as infection, hematoma, and partial necrosis of the flap. HBOT helps reduce these risks by promoting healing and inhibiting the growth of anaerobic bacteria, providing a safer recovery process for patients.
- Regression of edema and bruising: Swelling and bruising are common after facial surgery. HBOT can accelerate lymphatic reflux and reduce the accumulation of interstitial fluid, thus effectively relieving postoperative edema. At the same time, the hyperoxic environment also helps break down blood stasis and shortens the duration of bruising.
- Acceleration of recovery after liposuction: After liposuction, patients often experience swelling, pain, and tissue induration. HBOT can accelerate the relief of these symptoms by reducing inflammation and promoting tissue repair, allowing patients to return to daily activities more quickly.
Clinical Research Support:
We advocate evidence-based medicine, and the role of HBOT in healing after plastic surgery has been supported by multiple high-quality clinical studies and meta-analyses. These studies clearly show that HBOT can significantly shorten the recovery time of patients, reduce postoperative pain, improve the final aesthetic effect, and reduce the incidence of various complications. For example, studies have shown that patients receiving HBOT show a statistically significant advantage in wound healing speed; other analyses have shown that it can effectively reduce the incidence of complex wounds and infections.
List of potential benefits:
Taken together, patients with HBOT after plastic surgery can expect the following potential benefits:
- Accelerate wound healing: increase oxygen supply, promote collagen synthesis and angiogenesis.
- Reduce bruising and swelling: reduce inflammation, accelerate lymphatic reflux, promote blood stasis absorption.
- Reduce the risk of infection: high oxygen environment has inhibitory effect on anaerobic bacteria, and enhance the bactericidal ability of white blood cells.
- Improve the appearance of scars: By optimizing the healing process, it helps to form smoother and less obvious scars.
- Reduce postoperative pain: reduce inflammation and edema, thereby relieving nerve compression and pain.
- Shorter stay in hospital or rehabilitation center: Faster recovery means that patients can be discharged from the hospital more quickly and return to normal life.

When to Consider HBOT and Safety Precautions
In my clinical practice, patients or peers often ask whether hyperbaric oxygen therapy (HBOT) can be used after all plastic surgery? The answer is no. The application of HBOT requires great care and must be thoroughly evaluated by the attending physician.
Indications and contraindications:
We usually consider HBOT for those specific patients. For example, patients with a high risk of healing, such as diabetics, may have poor microcirculation per se; or patients with a history of past healing disorders, such as those with previously operated wounds that have been slow to recover or even infected. In addition, if a procedure itself is expected to have a high risk of complications, we may also consider HBOT as an adjunct, in the hope of optimizing the healing process and reducing unnecessary complications. We all hope that patients can recover as soon as possible and better.
Of course, there are indications for contraindications. There are some situations where HBOT is absolutely not allowed. For example, untreated patients with pneumothorax, this is a big taboo. Entering a high-pressure environment may lead to deterioration of pneumothorax, with disastrous consequences. Some patients with severe lung disease or ear infections also need to be cautious, because pressure changes may aggravate their condition or bring discomfort. Therefore, this is not something that can be decided casually. We will carefully consider the individual situation of every patient.
Importance of medical orders:
On this point, I really want to emphasize it again and again: HBOT must be conducted in a professional medical institution, and it must be guided and supervised by highly trained medical staff throughout the process. I’ve seen a lot of patients, and because I heard that HBOT works well, I thought about buying one myself “best hyperbaric chamber for home use”. This kind of thinking, I have to clearly point out the potentially huge risks.
Using a hyperbaric oxygen chamber at home on your own may sound convenient, but it’s actually extremely unrecommended. Think about it, professional HBOT treatment requires precise control of oxygen concentration, pressure, and treatment time, and there are professional healthcare workers monitoring the patient’s vital signs and response. If these are missing, you may be at risk for oxygen toxicity (rare though serious consequences), ear damage (resulting from an imbalance of stress), and even claustrophobic episodes. These are security risks that you cannot effectively deal with when operating at home.
If someone is really interested in “best hyperbaric chamber for home use benefits”, then be sure to keep in mind: this requires rigorous medical evaluation and professional guidance, and is generally not recommended as the primary or only option for postoperative recovery. Our medical professionals exist to ensure the safety and effectiveness of treatment, not to allow patients to take unnecessary risks.
Potential Risks and Side Effects:
Any medical intervention can come with risks, and HBOT is no exception. The most common side effect is ear pressure injury, like an uncomfortable ear when flying, but with professional ear pressure balancing techniques, it can usually be alleviated. Others may have sinus problems or transient visual changes. The most serious and most vigilant is the oxygen poisoning mentioned above. However, in a professional medical environment, through strict programs and monitoring, this risk is extremely low and can be basically avoided.
What to Expect During an HBOT Session

Process Overview:
Usually, when you decide to receive hyperbaric oxygen therapy as an auxiliary rehabilitation after plastic surgery, the first step is to make an appointment and perform a preliminary evaluation. We will carefully review your medical history and procedures to ensure that HBOT is safe and effective for you. After that, you will be asked to change the treatment clothes on pure cotton, because in the pressurized cabin, we must ensure that there are no synthetic materials that may generate static electricity.
The next step is to enter the “hyperbaric chamber. According to the equipment of our clinic, this may be a single cabin, just like a transparent space capsule, so that you have enough private space; it may also be a multi-person cabin, where you with other patients receive treatment together, just like sitting in a small cabin. Either way, we have professional technicians to assist you all the way into the cabin and ready.
Hyperbaric chamber environment:
After entering the Hyperbaric chamber and starting to pressurize, the most common feeling is the ear pressure change, which is very similar to the feeling when the plane is taking off and landing. We will guide you to do some simple movements, such as swallowing, yawning, or pinching your nose to shut up and exhale, to help balance the ear pressure. The temperature in the cabin will be kept in a comfortable range. You can relax and rest, or bring a book or tablet to read, watch a movie, or even take a nap. Our medical staff will communicate with you through the intercom system to ensure your comfort.
Frequency and duration of treatment:
The specific course of treatment depends to a large extent on your type of plastic surgery, recovery progress and individual response. Typically, each HBOT session lasts 60 to 90 minutes. As for frequency, some patients may require daily treatment, others several times a week. Importantly, these treatment packages must be tailored to your specific situation by your treating physician or hyperbaric oxygen specialist.
Treatment team:
You will be cared for by a professional medical team throughout your treatment with HBOT. This includes experienced doctors who will assess your condition and develop a treatment plan; well-trained HBOT technicians who are responsible for operating the hyperbaric oxygen chamber to ensure the safe and stable operation of the equipment; and, of course, careful nurses who will pay attention to your physical condition and provide necessary care and support. We know that a professional and empathic team is key to ensuring treatment outcomes and patient safety. After all, we want you to be safe and effective on your way to recovery.
Conclusion:
From physiological mechanisms to clinical practice, hyperbaric oxygen therapy has shown great potential in the management of recovery after plastic surgery. It can not only significantly improve the healing speed of the tissue, reduce the risk of swelling and infection, but also improve the quality of the scar, so that the surgical effect is more natural and lasting.
However, HBOT is not for everyone, nor is it a “home remedy” to try at will “. Only when evaluated by a professional doctor and implemented in a safe medical environment, can it truly play the greatest therapeutic value.
If you are planning or have just had plastic surgery, talk to your doctor about whether HBOT is right for you. Scientific, prudent and individualized postoperative management is the key to ensure smooth rehabilitation and ideal results.
Frequently Asked Questions About HBOT After Surgery:
Q : Is hyperbaric oxygen therapy safe after plastic surgery?
A : Yes — when performed in a certified medical facility under professional supervision, HBOT is considered very safe.
Common side effects such as mild ear pressure or temporary vision changes are usually short-term and easily managed.
It should never be done at home without medical oversight.
Q : How soon after surgery can I start hyperbaric oxygen therapy?
A : In most cases, patients can start HBOT within 24–72 hours after surgery, depending on the procedure and doctor’s assessment.
For reconstructive or flap surgeries, early intervention may help improve tissue survival and reduce swelling.
Q : How many HBOT sessions are usually needed for recovery?
A : Typical recovery protocols range from 5 to 20 sessions, each lasting about 60–90 minutes.
The exact number depends on factors such as surgery type, healing progress, and individual response to treatment.
References:
Turgut, B., et al. (2024). Experience of hyperbaric chamber usage in aesthetic plastic surgery practice for recovery and complication prevention. Aesthetic Plastic Surgery Journal. PubMed
Bennett, M. H., et al. (2015). Hyperbaric oxygen therapy for acute surgical and traumatic wounds. Cochrane Database of Systematic Reviews, CD008059. Cochrane Library
Kranke, P., et al. (2009). Hyperbaric oxygen therapy for chronic wounds. Undersea & Hyperbaric Medicine Journal, 36 (6), 433–457. PubMed
Celik, O., et al. (2022). Role of hyperbaric oxygen therapy in cosmetic and reconstructive surgery in ischemic soft tissue wounds: A case series. Aesthetic Surgery Journal Open Forum. PubMed
Wang, S., et al. (2024). Adjunctive hyperbaric oxygen therapy and negative pressure wound therapy for hard-to-heal wounds: A systematic review and meta-analysis. Journal of Wound Care. PubMed
Undersea and Hyperbaric Medical Society (2023). Hyperbaric oxygen therapy enhances autologous bone graft integration. Undersea & Hyperbaric Medicine Journal. UHMS







No Comment! Be the first one.